If you have booked a private skin cancer consultation — or are thinking about doing so — this guide is designed to demystify the appointment. Whether you have a lesion you are worried about, a referral letter from your GP (General Practitioner), or you simply want a baseline skin check, knowing what will happen tends to make the whole experience feel far smaller.
The short version: a good private skin cancer consultation is unhurried, diagnostic, and action-oriented. You should leave with a clear understanding of what you have, what it means, and what happens next.
Why patients choose the private pathway
Patients come privately for several reasons, and none of them is wrong:
- Speed of access. A private appointment can usually be offered within a few days, not weeks.
- Continuity of care. You see the same consultant from first assessment to surgery to follow-up. In busy NHS services, that continuity is not always possible.
- Time with the specialist. Initial private appointments are typically 30 minutes, which allows a full history, a complete skin examination and a proper discussion.
- Peace of mind. Many patients come for a single reassurance appointment and leave with a definitive answer about a lesion they have worried over for months.
Before your appointment: what to bring
A little preparation makes the appointment much more productive.
- Referral letter (if you have one) — useful but not essential.
- A list of your current medications, including any over-the-counter supplements and blood-thinning drugs such as aspirin, warfarin or DOACs (Direct Oral Anticoagulants).
- Your family history of skin cancer — particularly melanoma in first-degree relatives.
- Photographs of the area of concern, especially if you have noticed changes over time. A simple phone photograph with a ruler or coin for scale is genuinely helpful.
- A list of questions — it is surprisingly common to forget them in the moment.
"The most useful thing you can bring to a skin consultation is a clear story. When did you first notice it? What has changed? A two-line history often steers the diagnosis faster than any gadget."
The structure of the appointment
A typical private skin cancer consultation follows a predictable flow, though the emphasis shifts depending on your reason for attending.
1. History (10–15 minutes)
We start with a careful conversation. How long has the lesion been there? What has changed? Any symptoms — bleeding, itching, tenderness? What is your skin type, and how has your sun exposure looked across your life? Any family history of melanoma or non-melanoma skin cancer? Any relevant medical conditions or medications?
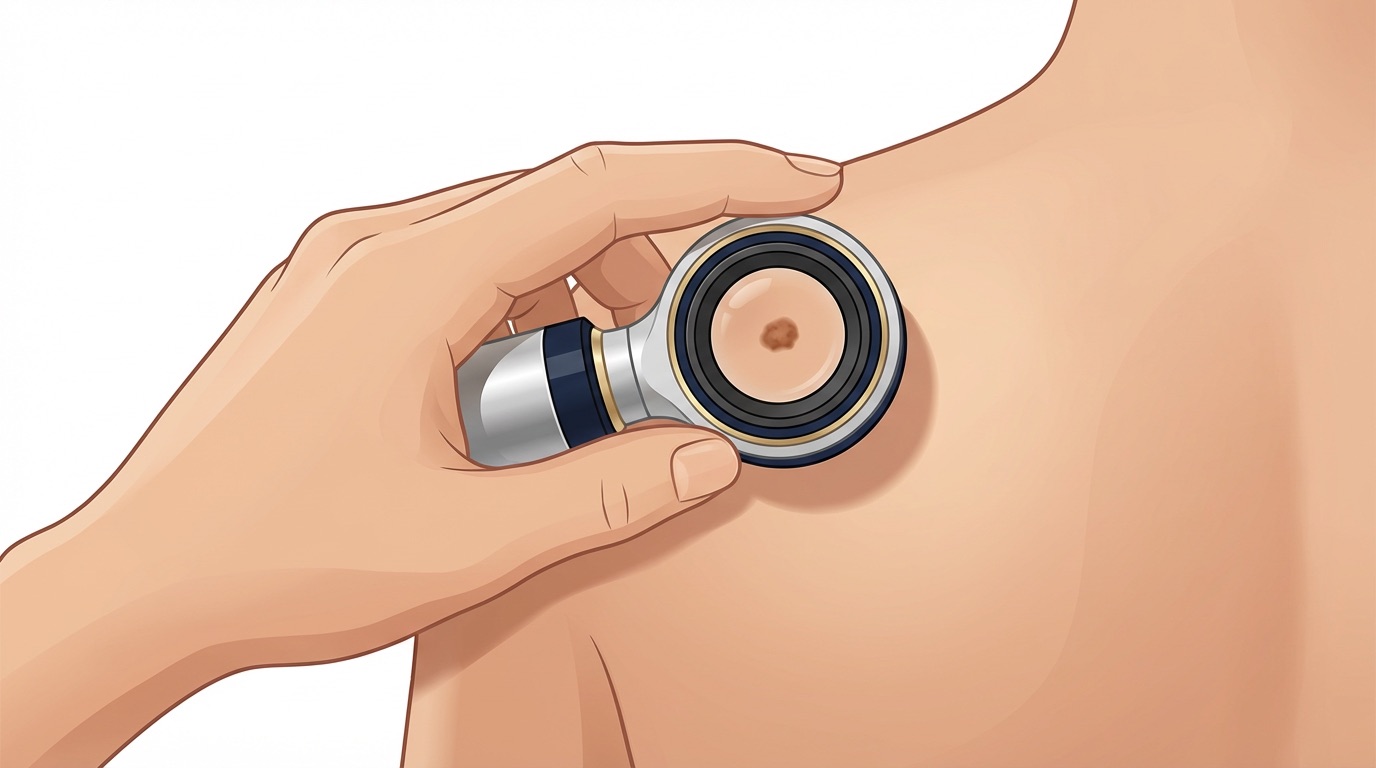
2. Skin examination and dermoscopy
I then examine the area of concern in good light, and — with your permission — the rest of the skin. A dermatoscope is used to magnify and polarise the lesion, revealing patterns invisible to the naked eye. Many lesions can be confidently diagnosed at this stage, avoiding the need for biopsy altogether.
3. Discussion and plan
We then sit down and talk through what has been found. If it is benign, you are discharged with reassurance and a plan for self-monitoring. If it is suspicious, we discuss biopsy or definitive excision — usually as a day case procedure, under local anaesthetic, if appropriate. If more information is needed first, we arrange it before treatment.
Investigations that may be arranged
- Biopsy under local anaesthetic: a small sample of the lesion (or the whole lesion) is removed and sent to the laboratory for histology. Results typically return within 7–10 working days.
- Imaging: in higher-risk tumours, ultrasound of the draining lymph nodes, or cross-sectional imaging — CT (Computed Tomography), MRI (Magnetic Resonance Imaging) or PET-CT (Positron Emission Tomography combined with CT) — may be arranged.
- Photography of moles for baseline documentation and future comparison.
Typical timescales
One of the main advantages of the private pathway is that each step is fast.
- First appointment: usually within 3–7 days of enquiry.
- Urgent biopsy: booked to happen as soon as possible.
- Histology results: typically within 1–2 weeks.
- Multidisciplinary team (MDT) discussion: for confirmed skin cancers, your case is discussed at a specialist MDT meeting attended by dermatologists, plastic surgeons, pathologists and oncologists.
- Definitive surgery: typically within 2–4 weeks of diagnosis.
Insurance and self-pay
The UK's major private medical insurers — including Bupa, AXA Health, Aviva, Vitality and WPA — cover skin cancer assessment, biopsy and treatment. I am recognised by each of these providers. If you are using insurance, please obtain a pre-authorisation code before your appointment — the insurance team at your hospital can help with this.
Self-pay is also straightforward. Transparent pricing is available for consultations, biopsies and common excisions, and written estimates are provided in advance of any treatment.
What happens if it's not cancer
Many patients who come worried about a lesion are reassured to find it entirely benign — a seborrhoeic keratosis, a dermatofibroma, a cherry angioma or a stable mole. In that case you will usually be discharged with clear self-monitoring advice and the option to return if anything changes. For patients with numerous moles or a personal or family history, an annual baseline skin check is often sensible.
Continuity between private and NHS care
Choosing a private consultation does not commit you to private treatment. If a skin cancer is diagnosed, you are always welcome to continue your treatment on the NHS, and I will arrange a prompt onward referral with a full summary of the assessment. Equally, patients under NHS care sometimes choose to transfer parts of their pathway — a biopsy, a follow-up appointment, or definitive surgery — to a private setting for speed or convenience. I am happy to liaise with your NHS team to ensure everything runs smoothly in either direction.
To arrange an appointment, please visit the contact page, explore our Skin Cancer Centre, or read more about the broader patient journey. If you would like a primer on warning signs before your appointment, our guide to the early signs of skin cancer and the article on when to worry about a mole are both useful starting points.