Keloid Scar Treatment
Keloid scars are raised, firm scars that grow beyond the boundaries of the original wound, often continuing to enlarge over time. Mr Singh offers a combined, individualised approach to keloid management using surgical excision, steroid injections, silicone therapy and, in selected cases, adjuvant radiotherapy to achieve the best possible long-term outcome.
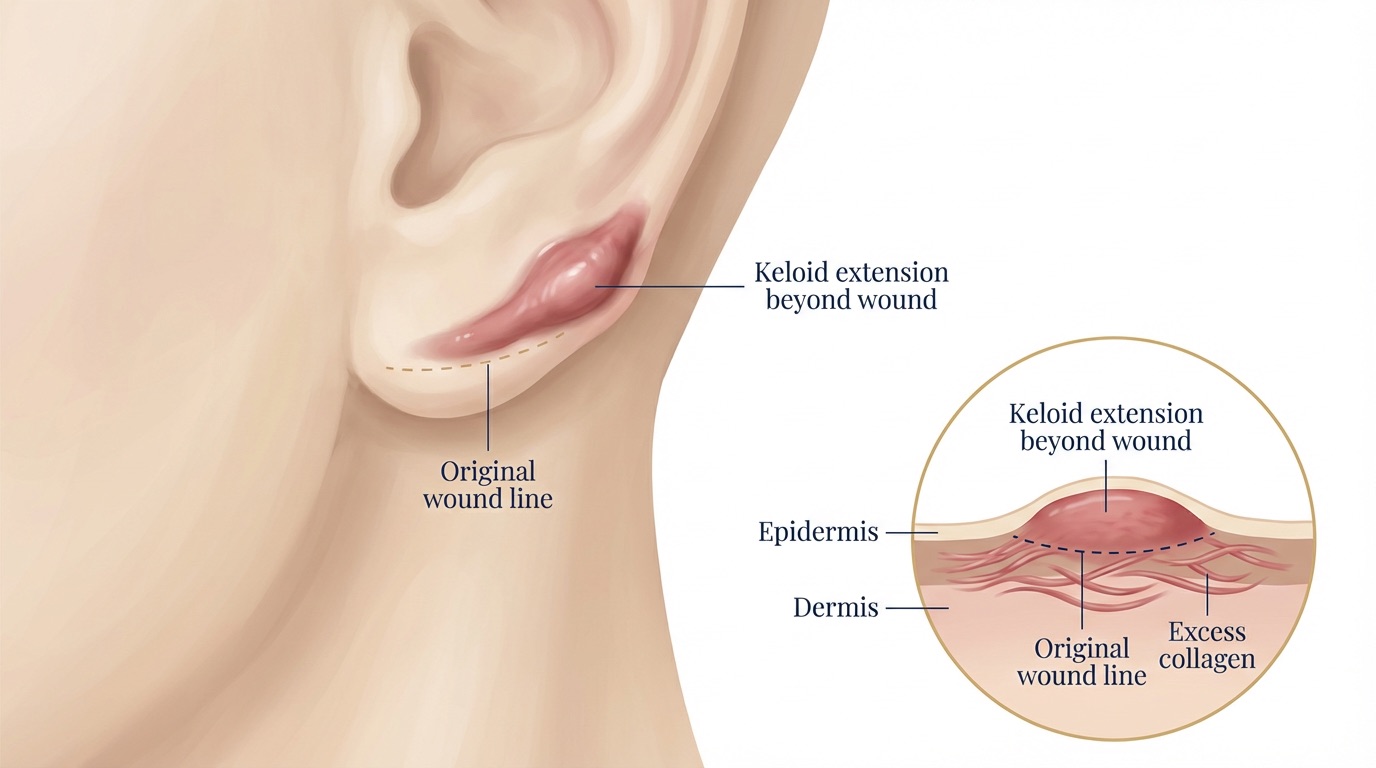
Overview
Keloid scars are a particular type of abnormal scar that extends beyond the borders of the original wound and does not regress over time. They are caused by an exaggerated and unregulated healing response, with excessive deposition of collagen in the skin. Keloids can arise from even minor skin injuries such as ear piercings, acne, vaccinations or surgical incisions and are more common in individuals with darker skin types and those with a family history of keloid formation.
Because keloids have a strong tendency to recur after simple removal, treatment is rarely a single step. Mr Singh adopts a combined, multi-modal strategy that is tailored to the size, location and behaviour of each keloid, often involving a combination of surgical excision, intralesional steroid injections, silicone therapy and, where appropriate, adjuvant radiotherapy to reduce the chance of recurrence.
Benefits
- Reduction in scar size: A noticeable flattening and shrinking of bulky, raised keloid tissue.
- Symptom relief: Improvement in the itching, burning, tenderness and pain often associated with active keloid scars.
- Improved appearance: A softer, less conspicuous scar that blends more naturally with the surrounding skin.
- Lower recurrence risk: The combined approach significantly reduces the high recurrence rate seen with simple excision alone.
- Restored function: Where keloids cross joints or limit movement, treatment can restore range of motion and flexibility.
- Psychological benefit: Enhanced self-confidence and comfort in clothing, particularly when keloids are in visible areas.
Surgical Techniques
Because keloids recur so readily, successful management usually requires more than one treatment modality. Mr Singh will assess the scar and devise a tailored plan that may combine several of the approaches below.
- Surgical Excision: The keloid is carefully cut out and the wound closed meticulously under local anaesthetic, usually avoiding tension and planning the scar along relaxed skin tension lines where possible.
- Intralesional Steroid Injections: Steroid is injected directly into the scar to soften it, reduce itch and tenderness and lower the risk of recurrence. A course of injections is typically required, spaced several weeks apart.
- Silicone Therapy: Medical-grade silicone sheets or gels are used following excision to hydrate the scar and reduce collagen overproduction during healing.
- Pressure Therapy: In suitable sites such as the ear lobe, custom pressure clips or garments are used to discourage recurrence after excision.
- Adjuvant Radiotherapy: For large or high-risk keloids, a short course of superficial radiotherapy immediately after surgical excision can substantially reduce recurrence rates. This is arranged with a clinical oncology colleague when appropriate.
- Combination Protocols: Most patients benefit from a staged plan that combines surgery with injections and silicone, with careful monitoring during the first year when recurrence risk is highest.
Risks & Considerations
General Risks
- Infection: Any wound carries a small risk of infection which may delay healing and require antibiotics.
- Bleeding and bruising: Minor bleeding or bruising can occur at the excision or injection site.
- Scarring: All treatments leave some form of scar; the aim is to achieve a flatter, less symptomatic result.
- Anaesthetic reactions: Rare local anaesthetic reactions or discomfort during injection.
Specific Risks to Keloid Treatment
- Recurrence: Despite a combined approach, keloids can recur and further treatment may be required. Close follow-up in the first year is essential.
- Skin atrophy and depigmentation: Steroid injections can thin the surrounding skin and cause lightening or darkening of pigmentation, particularly in darker skin types.
- Telangiectasia: Small dilated blood vessels can appear in and around injected skin.
- Radiotherapy effects: Where used, superficial radiotherapy can cause local skin changes and, very rarely, carries a theoretical long-term risk of secondary skin malignancy.
- Unpredictable response: Individual keloids behave differently; some respond rapidly, others require prolonged treatment over many months.
- Wound dehiscence: Separation of the excision wound, especially in high-tension sites such as the chest or shoulders.
Recovery
Wound Care
- Dressings: A simple dressing is applied after excision and usually kept in place for the first few days; it is designed to tolerate gentle showering.
- Cleaning: Once the dressing is removed, the wound can be gently cleaned with mild soap and water and patted dry. Daily showering is encouraged to reduce infection risk.
- Activity: Most daily activities can be resumed straight away, though heavy lifting and vigorous exercise should be avoided for around two weeks to protect the wound.
Scar Advice
- Silicone Therapy: Silicone sheets or gels should be started once the wound is fully healed and continued for several months to reduce the risk of recurrence.
- Sun Protection: New scars must be protected from sun exposure with high-factor sunscreen or clothing for the first 6–8 weeks.
- Scar Massage: Once the wound is healed, regular gentle massage with moisturiser helps to soften the scar and improve its texture.
- Pressure and Injections: Ongoing pressure therapy or steroid injection appointments may form part of your recovery plan to maintain the result.
Follow-Up
- Initial Post-Op Visit: Typically scheduled around a week after excision to check wound healing. Sutures are usually dissolving.
- Injection Appointments: Steroid injections are commonly given at 6 to 8 week intervals over several months to maintain softness and control recurrence.
- Medium-Term Review: Further reviews at 3, 6 and 12 months allow Mr Singh to monitor for any early signs of recurrence and adjust treatment as required.
- Long-Term Care: Mr Singh remains available for any concerns or further follow-up as required, particularly during the first year when recurrence risk is highest.
Procedure Summary
Ready to Discuss Keloid Scar Treatment?
If you are troubled by a keloid scar and would like to explore a tailored combined treatment plan, please contact us to answer any questions you may have or to schedule a consultation with Mr Singh.
Book a Consultation